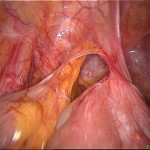
 If a patient has chronic abdominal pain, a feeling of fullness, trapped gas, nausea, vomiting, constipation, or obvious difficulty in the movement of food through their gut, then they may have developed intestinal adhesions. Adhesions are the most common cause of intestinal obstruction.
If a patient has chronic abdominal pain, a feeling of fullness, trapped gas, nausea, vomiting, constipation, or obvious difficulty in the movement of food through their gut, then they may have developed intestinal adhesions. Adhesions are the most common cause of intestinal obstruction.
In a healthy person the intestine is free to move inside the abdominal cavity and is in constant motion, writhing around like a bag of worms. The intestine is very slippery and this allows the loops of gut to move freely over one another as food moves through them from place to place. The loops naturally slide away from areas which more full and are taking up more space.
If there has been a source of chronic inflammation inside the body cavity then this may encourage the formation of bands of scar tissue that attach the outside surface of one loop of intestine to neighboring loops or to the inside wall of the abdomen. As a result, parts of the gut are tied together or pinned in place. This prevents them from moving and potentially makes it more difficult for food to find a way through as the intestines try to move around. Intestinal loops may kink or twist blocking the flow. As a result loss of normal gut motion occurs and partial or full obstruction develops. Most of the time the twisting is intermittent, but occasionally the twisting does not reverse spontaneously. If the blood supply is restricted, this might result in a crisis where the gut is damaged.
Full gut obstructions lead rapidly to vomiting and extreme pain with the inability to eat and drink and is a medical emergency, often requiring surgery. Obstruction is diagnosed using an X-ray or CT scan. In the case of the chest X-ray the classical sign of this condition is the “levels” sign, where it is possible to see horizontal standing fluid levels at multiple locations in the gut. On the CT scan the gut may be abnormally dilated by trapped fluid.
More limited adhesions can lead to recurring partial obstruction with less extreme symptoms, but a lack of proper drainage of the bowel.
Common reasons for adhesions are previous abdominal surgery and prolonged appendicitis. During surgery the gut can be easily irritated by being exposed to the air or by being handled. This can encourage inflammation which can cause the growth of scar tissue. A person can also have an appendix which has repeatedly become inflamed and then recovered without causing a sufficient crisis for removal. This inflammation can irritate neighboring tissues, including the intestine or peritoneal lining of the abdominal cavity and also encourages the formation of scar tissue. Scar tissue may take months or years to develop.
In autopsy studies, adhesions were found to be spontaneously present in about 28% of individuals who had never had any abdominal surgery, but the incidence can rise as high as 93% after multiple surgeries. A meta-analysis showed that 51-66% of people typically formed adhesions after abdominal surgery, depending on the kind. Laparoscopic methods reduced the adhesion formation rate. However it’s important to note that many adhesions are benign and cause no symptoms.
In women, adhesions can also involve the uterus or fallopian tubes and lead to infertility.
Adhesions of the gut to the peritoneum can cause pain and a feeling of tension or pulling in the abdomen.
Typical symptoms of obstruction involve abdominal discomfort around the belly button that feels like cramping, and also distention of the belly. Symptoms typically get worse with eating and there may be a reduction in the passing of gas or stool. Nausea and vomiting develop with severe obstruction. However most adhesions do not cause symptoms.
The only treatment for adhesions is surgery. Patients undergo either laparoscopic or open surgery and the bands of scar tissue are cut by a scalpel or by electrical current. Unfortunately adhesions have a tendency to re-form and any interference with the gut during surgery encourages adhesions. Laparoscopic surgery is the best option because it is less invasive, but the risks of surgery have to be balanced with quality of life issues.
If a patient is dealing with partial obstructions then a liquid diet may help, or alternatively the consumption of small frequent meals.
Alternative therapies that target adhesions include the use of castor oil packs, doing regular yoga or abdominal stretching exercises, visceral massage, and taking the supplement serrapeptase which is an enzyme that is intended to slowly dissolve scar tissue. These therapies are entirely based on anecdotal evidence and may be ineffective.
