 An upper endoscopy is usually ordered by a gastroenterologist if a patient is experiencing upper abdominal digestive discomfort, nausea, vomiting, problems swallowing, or acid reflux. It can be used to check the state of the esophagus, stomach, and duodenum for growths, cancer, inflammation, and ulcers, as well as any physical abnormality.
An upper endoscopy is usually ordered by a gastroenterologist if a patient is experiencing upper abdominal digestive discomfort, nausea, vomiting, problems swallowing, or acid reflux. It can be used to check the state of the esophagus, stomach, and duodenum for growths, cancer, inflammation, and ulcers, as well as any physical abnormality.
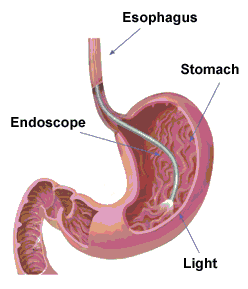
The physician uses an endoscope with a camera that allows the interior of the stomach to be viewed. Attachments are available to retrieve tissue samples for laboratory examination.
Preparation for the study involves refraining from eating or drinking for a number of hours before the appointment in order to ensure that the stomach is empty and that the patient is in a safe condition for the administration of sedative drugs.
Typically the patient is given drugs to relieve them of pain, inhibit the gagging reflex, and sedate them so that they barely remember anything from the procedure. The anesthetic level is sufficiently light so that the patient is able to be cooperative during the procedure.
Once anesthetized, the patient is asked to swallow the probe. This part is barely remembered after the procedure and is not normally problematic. The endoscope is passed down the esophagus into the stomach, and eventually through the pyloric sphincter, and into the first part of the duodenum. The distance that can be examined is limited. The probe is not typically able to pass very far into the small intestine, but it is possible to check for ulceration in the stomach and duodenum, and possible for obstruction of the bile ducts in the case of an endoscopic retrograde cholangiopancreatogram (ERCP).
It is normal to experience a sore throat following this procedure.
